Tuesday, November 29, 2022
Screening for Adverse Childhood Experiences is Increasing, but are Patients Getting Treatment?
Posted By Elizabeth Aguilera, CALmatters on Tue, Nov 29, 2022 at 9:08 AM
Today the number of doctors screening patients for adverse experiences is growing, but the state is failing to track whether patients receive the follow-up services or support they might need. State officials say they are working on identifying this information about patients from state medical databases, but it could be a few years off.
More than 6 in 10 Californians have experienced at least one adverse childhood experience, and 1 in 6 have experienced four or more, according to a state report. These include physical, emotional or sexual abuse, physical or emotional neglect, growing up in a home with substance use, mental illness, incarceration, parental separation or divorce or intimate partner violence. Research shows the higher the number of adverse experiences, the higher the risk of chronic health or mental health conditions later in life.
Since the Office of the California Surgeon General began the program, about 900,000 children and adults on Medi-Cal, the state’s health insurance plan for low-income people, have been screened. The program, known as ACEs Aware, tracks only the screenings done by Medi-Cal doctors who choose to incorporate them into their practice. Medi-Cal reimburses providers $29 per screening. Last year, the state mandated private insurers pay for screenings too, but the state does not require or track those.
After screening a patient, physicians may make referrals to therapists, nutritionists, social workers and other support services. A score of four adverse childhood experiences is used as a marker for doctors to offer referrals but they assess patients based on a wide variety of factors. They may make referrals for someone with one adverse experience or only talk with someone with six adverse experiences because they have been able to buffer their experiences.
Physicians aren’t required to report whether patients receive support services or if the services are available to them. That’s part of the challenge. The state’s serious shortage of mental health professionals, social workers and other support health care workers, like nutritionists and physical therapists, makes it even harder for physicians to make referrals and for patients to get help.
“Right now, with our patients, we give them a referral or a list of options/therapists,” said Reshmi Basu, a pediatrician and president-elect of the American Academy of Pediatricians – Orange County Chapter. “But once we do that, we don’t know what happens. We don’t know if they are taking new patients.”
Monday, November 28, 2022
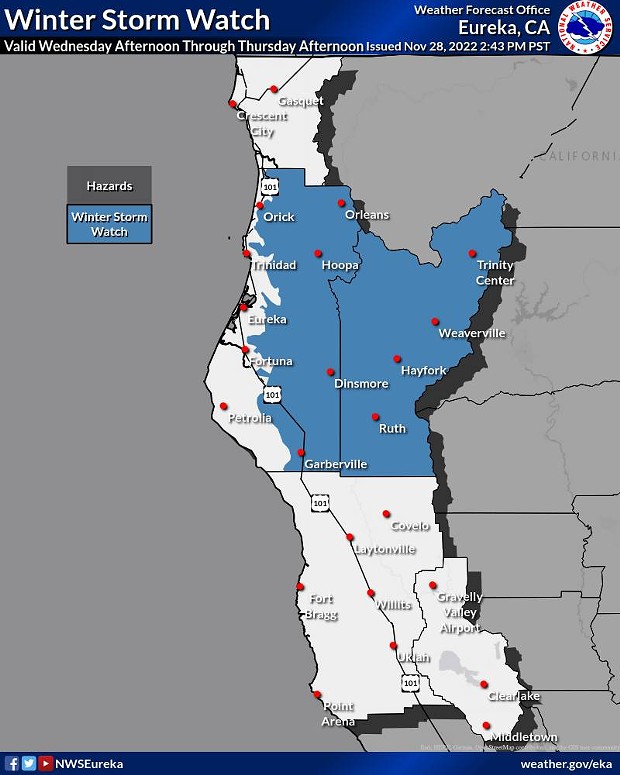
Frigid Temps on the Coast Tonight, Winter Storm Watch in the Interior Wednesday
Posted By Kimberly Wear on Mon, Nov 28, 2022 at 3:01 PM
"Heavy snow possible above 2,000 feet," the weather message states. "Total snow accumulations of 7 to 24 inches possible. Winds could gust as high as 40 mph."
The NWS notes that travel on mountain roads and passes "could be very difficult to impossible" and "hazardous conditions could impact the morning or evening commute."
Meanwhile, coastal areas stretching from Del Norte to Mendocino will be under a freeze warning effective at midnight and running to 9 a.m. Tuesday, with temperatures dipping down into the mid-20s in some area, according to NWS.
Wednesday, November 23, 2022
Latest Election Results: Cervantes Takes the Win, Earth Flag Appears Ready to Fly High
Posted By Kimberly Wear on Wed, Nov 23, 2022 at 11:50 AM
With no real changes overall, the two big flips — the Ward 3 seat on the Eureka City Council and the Earth flag measure in Arcata — continued the course of last week's results.
Meanwhile Juan Pablo Cervantes, ahead by 4,800 votes, maintained his lead over Tiffany Hunt Nielsen and is now slated to become Humboldt County's next clerk/recorder/registrar of voters with a solid 56.1 percent of the vote.
Over in the Third Ward, G. Mario Fernandez kept his momentum after pulling ahead of John Fullerton last week, taking 53 percent of the vote. The two are separated by 118 votes.
In Arcata, Meredith Matthews and Kimberley White, who have overwhelmingly dominated the race for two open seats in a field of six candidates, will take their place at the dais Dec. 15 to form the city's first ever all-woman city council after taking 35 percent and 34 percent of the vote, respectively.
Also in Arcata, voters look to have given the nod to placing the Earth flag atop city owned flagpoles, with Measure M keeping its slight 51 percent lead.
This latest round brings voter turnout to 55 percent of those registered. To find all of the results click here.
Laytonville Resident Killed in 101 Crash
Posted By Iridian Casarez on Wed, Nov 23, 2022 at 10:18 AM
According to a CHP release, a Toyota 4Runner heading northbound just before 4 p.m., driven by Beatriz Diaz-Rodriguez, struck a Subaru Impreza driven by Zora Culps head-on.
"For reasons still under investigation, the Toyota crossed from the northbound lane over the solid double yellow divider lines into the southbound lane into the direct path of the Subaru."
Diaz-Rodriguez, 34, died from her injuries at the scene while Culps, 20, sustained major injuries and was transported to St. Joseph's Hospital for further medical care.
It's still unknown if drugs or alcohol were a factor in the collision. The crash is still under investigation by the Garberville CHP.
Tuesday, November 22, 2022
Multiple Dogs in Cutten Die from Possible Poisoning
Posted By Iridian Casarez on Tue, Nov 22, 2022 at 5:11 PM
According to a sheriff's office news release, multiple dogs have died after reportedly exhibiting symptoms associated with poisoning. A preliminary investigation found the dogs may have consumed an unknown green substance found on the sidewalks of the neighborhood.
Residents living near Excelsior Road in Cutten are encouraged to inspect their yards and sidewalks for any unknown materials and keep a close eye on their pets when out on walks in the area.
Lead Ammo in Poached Elks Could Have Killed Condors
Posted By Kimberly Wear on Tue, Nov 22, 2022 at 4:24 PM
According to a release from the Northern California Condor Restoration Program — a partnership between the Yurok Tribe and Redwood National and State Parks — one of the carcasses discovered Nov. 12 “contained enough lead to kill several condors.”
“This is about as close as you can get to a worst-case scenario. If the carcasses weren’t quickly reported, and our free-flying condors accessed them, it is very likely that one or more of the condors would have consumed a life-threatening quantity of lead,” said NCCRP Manager and Yurok Wildlife Department Manager Chris West, who has more than two decades of condor management experience. “The risk this incident presented to the condors cannot be understated, since at least four of our recently released condors were less than a 10-minute flight from the poaching event at the time that it occurred.”
The release states the poaching case is being investigated by officers with Redwood National and State Parks and the California Department of Fish and Wildlife. Anyone with information is urged to come forward by calling NPS Ranger Attendorn at (707) 465-7789 or Game Warden Castillo at (707) 673-3678. Anonymous reports can also be made to the CDFW CalTip at (888) 334-CalTIP (888 334-2258) or by calling the park’s crime tip line at (707) 765-7353.
“Based on the circumstances, we’re lucky we didn’t have to transport condors for treatment or lose a bird to lead poisoning,” said Yurok Wildlife Department Director Tiana Williams-Claussen, who spent most of her adult life working to fulfill a council of Yurok elders’ wish to bring back the bird they hold sacred and know as prey-go-neesh to its historic territory. “Lead is by far the single biggest threat to condors in the wild.”
Known as nature’s clean-up crew, condors play an important role in the ecosystem as apex scavengers that use their powerful beaks to pierce the tough skins of dead animals ranging from elk to sea lions and even the occasional whale, clearing the large carcasses from the landscape and helping to prevent the spread of disease.
This makes the massive birds with a nearly 9-foot wingspan highly susceptible to lead poisoning from ammunition. In this case, the NCCRP states “several lead fragments, including the bulk of the lead ammunition round, were found in the neck of one of the cow elk and within a fist-sized chunk of meat presumably dropped by the poachers at the site.”
Since being reintroduced into the wild, about half of the condor deaths have been attributed to the birds eating lead fragments in animal carcasses.
“In general, when a condor consumes lead fragments, the bird will experience a series of worsening symptoms that often unfold over the course of days and weeks and lead to an excruciating death,” the release states.
FBI Takes on Fair Association Embezzlement Investigation
Posted By Thadeus Greenson on Tue, Nov 22, 2022 at 8:03 AM
Nina Tafarella, 47, was arrested Nov. 15 by Ferndale police at Bear River Casino on suspicion of embezzling more than $20,000 from a Eureka nonprofit that provides youth enrichment programs and an untold sum from the fair association. But Sligh said that after conferring with the FBI, the Humboldt County District Attorney's Office and Eureka police, "we decided the FBI will take the lead on it and prosecute federally."
Sligh said the decision was made because the FBI and the U.S. Attorney's Office of Northern California have more experience with financial crimes.
Tafarella, who has not been charged with a crime stemming from her arrest, was released from jail on her own recognizance Nov. 18, according to Humboldt County Sheriff's Office online records.
The case spawned out of Eureka, where, according to EPD spokesperson Brittany Powell, police believe Tafarella embezzled approximately $23,000 from a nonprofit that provides youth arts programs. Powell said the embezzlement is believed to have taken place over the course of about a year beginning in February of 2021 through Tafarella's capacity as a bookkeeper for the nonprofit. EPD had been investigating the case since late May, Powell said, and obtained a warrant for Tafarella's arrest Nov. 1.
Sligh said he first became aware of EPD's case around Nov. 10 when contacted by Humboldt County Fair Association General Manager Rich Silacci, who reached out after learning of the warrant for Tafarella, who'd also been serving as the association's bookkeeper since February of 2021. Silacci reported that Tafarella worked at the association and had access to its finances. Sligh said the fair association began an audit of its books, noticed discrepancies and what he believes is evidence Tafarella embezzled from it, too.
Officials have declined to say how much they believe was taken from the fair association, which has long struggled to gain a complete, accurate picture of its finances and has not had an external audit done since 2011.
In October of 2021, fair administrator Katherine Ziemer, wrote the board of directors on the subject of the fair's finances, saying she understood and shared directors' frustration on the subject. In the letter, Ziemer notes the association had hired a "very capable bookkeeper" who was working to get up to speed on the "fair-specific knowledge" needed to make sense of the organization's finances, which have been described as "extremely complex, with a 12-page listing of sub accounts."
Tafarella's hire also came at a point when the fair association was struggling financially and teetering on the edge of insolvency amid the pandemic, kept afloat by an influx of hundreds of thousands of dollars in COVID relief funds and a county grant.
As to the ongoing investigation, Sligh said he appreciates the assistance of the FBI, the DA's Office and EPD. Moving forward, Sligh said Ferndale police will assist if asked but the federal agencies will take the lead of both Eureka and Ferndale's investigations.
Monday, November 21, 2022
Sunny Skies for Holiday Week but Sneaker Waves Possible Turkey Day
Posted By Kimberly Wear on Mon, Nov 21, 2022 at 11:00 AM
The coast will see mostly cloudy to mostly sunny skies over the week (although there is a slight chance of showers Tuesday) with highs in the high 50s to low 60s, peaking on Thursday, followed by a chance of rain after 10 p.m. Friday and over the weekend, with rain currently set for likely on Sunday. Night temps will be in the low 40s.
Inland, meanwhile, is slated to see some unseasonably warm days, ranging from the mid-60s to low 70s with mostly sunny skies for most of the week before, too, having temperatures start to taper off by Friday and following the same course as the coast on the rain front. Chilly nights in the low 40s are also forecast.
But if a walk on the beach is in the plans for Thursday, you might want to make different plans as the Eureka office of the National Weather Service states a “mid- to long-period swell will create a risk for sneaker waves along the area beaches” that day.
Friday, November 18, 2022
Election Results Update: Fernandez Pulls Ahead in Eureka, Earth Flag Measure Gains Ground
Posted By Kimberly Wear on Fri, Nov 18, 2022 at 12:07 PM
With another 9,614 ballots counted, some leads widened while others shrank slightly, but overall the votes fell along the same lines as election night.
Meanwhile, Juan Pablo Cervantes strengthened his lead over Tiffany Hunt Nielsen to become Humboldt County's next clerk/recorder/registrar of voters with a solid 56.1 percent of the vote.
In Eureka, the race for city council flipped for the Ward 3 seat with G. Mario Fernandez at 52 percent of the votes leading John Fullerton's 48 percent. The two are separated by 78 votes.
Over in Arcata, Measure M, which would place the Earth flag in the top spot on city-owned flagpoles, gained some ground, with the no vote now ahead by just 54 votes.
The freshly counted ballots bump up turnout to 43.7 percent of registered voters. Another 10,000 or so still need to be counted.
See the latest election results here.
Slashing Greenhouse Gases: California Revises Climate Change Strategy
Posted By Nadia Lopez/CalMatters on Fri, Nov 18, 2022 at 10:09 AM
If adopted by the air board at its Dec. 15 meeting, the plan would radically reshape California’s economy, alter how Californians’ vehicles, buildings and appliances are powered, and ultimately serve as a blueprint for other states and countries to follow.
“Failure is not an option,” said air board Chair Liane Randolph. “There is too much at stake and we need to move as fast and as far as we can to lessen the worst impacts of climate change and leave future generations a livable and healthy California.”
The five-year climate change strategy, called a scoping plan, outlines in its 297 pages how California could end its reliance on oil and also clean up the nation’s worst air pollution.
The staff’s final draft plan adds bolder commitments, reducing fossil fuel use by 94 percent from 2022 levels by 2045 — up from a goal of 91 percent in the September version of the plan.
The plan also sets a more aggressive goal of cutting carbon emissions 48 percent below 1990 levels by 2030 – up from the 40 percent by 2030 required under state law — until reaching net-zero emissions in 2045. (Net-zero or carbon neutrality means striking a balance between the carbon dioxide added to the air and the carbon that’s removed.)